MRI Ordering Guide: A Comprehensive Overview (Updated 04/08/2026)
Navigating MRI ordering requires balancing patient needs with cost-effectiveness and appropriateness, especially considering rising healthcare expenses and potential delays in diagnosis․
Magnetic Resonance Imaging (MRI) is a powerful diagnostic tool, but appropriate utilization is crucial for optimal patient care and responsible healthcare spending․ This guide provides a comprehensive overview of the MRI ordering process, aiming to equip clinicians with the knowledge to make informed decisions․ Traditional imaging centers often present challenges like lengthy wait times and complex scheduling, potentially delaying critical diagnoses․
However, advancements are streamlining access, with some facilities offering direct access MRI options, eliminating the need for a prior referral in certain situations․ Understanding state-specific regulations regarding referrals is paramount․ Effective MRI ordering necessitates integrating clinical findings with established guidelines, such as the American College of Radiology (ACR) Appropriateness Criteria, ensuring the examination is truly indicated and will yield valuable diagnostic information․ This guide will explore these facets and more․
Understanding the Need for an MRI
Determining whether an MRI is the appropriate imaging modality requires careful consideration of the clinical question and potential benefits versus risks․ Judicious ordering is essential, given rising healthcare costs and limited resources․ While MRI excels in soft tissue visualization, it’s not always the first-line investigation․ A systematic review highlights that CT scans and conventional radiography remain frequently utilized imaging modalities․
Evaluating the patient’s symptoms, physical examination findings, and relevant medical history is paramount․ Furthermore, understanding the impact of imaging referral guidelines on both patient care and radiology services is vital; Appropriate utilization focuses on high-value imaging, ensuring the scan provides clinically relevant information that will directly influence patient management․ Considering alternatives is a key component of responsible ordering․
2․1 When is an MRI Necessary?
MRI becomes necessary when detailed soft tissue assessment is crucial for diagnosis, particularly when other modalities are insufficient․ Neurological conditions like suspected stroke, multiple sclerosis, or spinal cord abnormalities frequently warrant MRI․ Musculoskeletal injuries, especially those involving ligaments, tendons, or cartilage, often benefit from MRI’s superior visualization․
Abdominal and pelvic pain of unclear origin, or suspicion of organ pathology, may also necessitate an MRI․ Cardiac MRI is indicated for evaluating heart structure and function․ However, it’s vital to remember that MRI isn’t always the immediate answer; clinical judgment, guided by established appropriateness criteria, dictates the need․ Delays in diagnosis should be avoided, and direct access options can expedite the process․
2․2 Alternatives to MRI: Considering Other Imaging Modalities
Before ordering an MRI, consider alternative imaging options based on clinical presentation and diagnostic goals․ X-rays are often the first line for bone injuries, offering quick and cost-effective assessment․ Computed Tomography (CT) excels at visualizing bone detail and detecting acute hemorrhage, but involves ionizing radiation․ Ultrasound is valuable for soft tissue evaluation, particularly in real-time, and avoids radiation exposure․
The choice depends on the specific clinical question․ For instance, while MRI is superior for ligament tears, an X-ray might suffice for a simple fracture․ Evaluating imaging volumes reveals that CT and radiography are frequently used․ Prioritizing appropriate imaging, guided by guidelines, minimizes unnecessary MRI scans and associated costs․
The Role of Referral Guidelines
Imaging referral guidelines are crucial for optimizing patient care and resource utilization․ They aim to ensure MRI scans are ordered appropriately, reducing unnecessary examinations and associated costs․ These guidelines impact both patient outcomes and the efficiency of radiology services, influencing imaging volumes and the proportion of high-value imaging performed․
Implementing guidelines can improve the appropriateness rating of imaging decisions․ Utilizing established criteria, such as those from the American College of Radiology (ACR), provides a standardized framework for clinicians․ This structured approach supports informed decision-making, promoting judicious MRI ordering and enhancing the overall quality of diagnostic imaging pathways․
3․1 Impact of Imaging Referral Guidelines on Patient Care
Effective imaging referral guidelines directly influence the speed and accuracy of patient diagnoses․ By reducing unnecessary scans, guidelines minimize patient exposure to radiation and potential delays in receiving appropriate treatment․ A systematic review highlights that guidelines impact imaging volumes, with the goal of increasing the proportion of truly appropriate examinations․
Improved guideline adherence can lead to earlier and more accurate diagnoses, ultimately enhancing patient outcomes․ Furthermore, optimized imaging pathways contribute to more efficient healthcare delivery, reducing wait times and streamlining the diagnostic process․ This is particularly important in musculoskeletal injury cases, where appropriate MRI referrals are vital for timely intervention and rehabilitation․
3․2 Utilizing the American College of Radiology (ACR) Appropriateness Criteria
The American College of Radiology (ACR) Appropriateness Criteria serve as a crucial decision support tool for clinicians ordering MRI scans․ These evidence-based guidelines integrate clinical findings with established imaging protocols, helping to determine the most suitable imaging modality for a specific clinical scenario․
Judicious MRI ordering, guided by ACR criteria, is essential for patient-centered care, especially given rising healthcare costs and limited resources․ Utilizing these criteria ensures that MRI scans are performed only when clinically indicated, minimizing unnecessary exposure and optimizing diagnostic yield․ Clinicians must thoughtfully integrate patient history, physical examination findings, and ACR recommendations to make informed decisions․
Direct Access MRI: Do You Need a Referral?
Traditionally, an MRI required a physician’s referral, but direct access MRI is increasingly available, offering patients greater control over their healthcare journey․ However, regulations vary significantly by state, impacting whether a referral is mandatory․ Many patients face lengthy waits and scheduling complexities with traditional imaging centers, delaying crucial diagnoses․
Concierge radiology services are emerging to address these challenges, providing quick and simple access to MRI scans, often without requiring a referral․ This convenience reduces wait times and empowers patients to proactively manage their health․ Understanding your state’s specific regulations is vital before scheduling a direct access MRI, ensuring compliance and avoiding potential issues with insurance coverage․
4․1 State-Specific Regulations Regarding MRI Referrals
MRI referral requirements are not uniform across the United States; they are determined at the state level, creating a complex landscape for patients and providers․ Some states mandate a physician’s referral for all MRI scans, while others permit direct access under certain conditions․ These conditions often relate to the patient’s insurance plan or the specific type of MRI being requested․
It’s crucial to verify the regulations in your state before scheduling an MRI, as non-compliance can lead to claim denials or the need to obtain a retroactive referral․ Resources like state medical boards and insurance providers can offer accurate, up-to-date information․ Direct access policies aim to streamline care, but navigating the varying state laws remains essential for a smooth process․
4․2 Benefits of Direct Access MRI: Reduced Wait Times & Convenience
Direct access MRI offers significant advantages, primarily in reducing the often lengthy delays associated with traditional referral-based systems․ Patients can bypass the scheduling hurdles and potential insurance conflicts that frequently plague conventional imaging centers, potentially waiting weeks or months for an appointment․ This expedited access is crucial for timely diagnoses and treatment initiation․
Furthermore, direct access enhances convenience by empowering patients to take a more active role in their healthcare․ It simplifies the scheduling process, eliminating the need for multiple appointments and paperwork․ This streamlined approach benefits both patients seeking prompt care and healthcare providers aiming for efficient workflows, ultimately improving patient outcomes․
Clinical Indications for MRI – By Body System
MRI’s versatility allows for detailed imaging across numerous body systems, guiding appropriate utilization․ Neurological MRI excels in evaluating brain tumors, strokes, spinal cord injuries, and nerve compression․ Musculoskeletal (MSK) MRI is invaluable for assessing joint injuries, muscle tears, and bone abnormalities, often utilized when GPs seek clarity on injury severity․
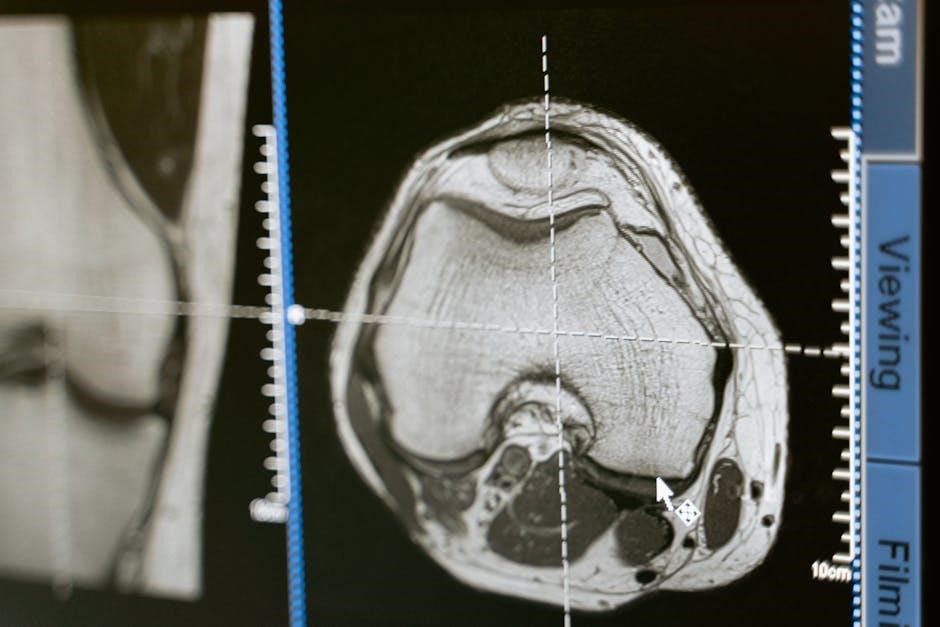
Abdominal and pelvic MRI aids in diagnosing organ pathologies, identifying tumors, and evaluating pelvic pain․ Cardiac MRI provides detailed views of the heart and blood vessels, crucial for assessing heart disease and congenital defects․ Judicious ordering, integrating clinical findings with guidelines like the ACR Appropriateness Criteria, is essential for maximizing benefit and minimizing unnecessary exposure․
5․1 Neurological MRI: Brain, Spine, and Nerves
Neurological MRI is paramount for diagnosing a wide spectrum of conditions affecting the central and peripheral nervous systems․ Brain MRI excels in detecting tumors, strokes, multiple sclerosis plaques, and congenital anomalies․ Spinal MRI is crucial for identifying herniated discs, spinal stenosis, and spinal cord compression, often following trauma or chronic pain․
Nerve MRI aids in evaluating nerve entrapment, injuries, and tumors․ Specific protocols, like diffusion-weighted imaging (DWI) for stroke, enhance diagnostic accuracy․ Consideration of clinical presentation alongside imaging findings is vital․ Appropriate use, guided by ACR criteria, ensures optimal patient care and avoids unnecessary scans․
5․2 Musculoskeletal (MSK) MRI: Joints, Muscles, and Bones
MSK MRI is indispensable for evaluating joint injuries, soft tissue damage, and bone abnormalities․ It’s frequently used for diagnosing ligament and tendon tears, cartilage damage (meniscal tears), and bone fractures not readily visible on X-rays․ MRI excels in visualizing muscles, identifying strains, contusions, and masses․

However, judicious ordering is key, as overuse exists․ GP training and quality assurance initiatives are crucial for appropriate referrals, particularly with direct access pathways․ Guidelines emphasize correlating clinical findings with imaging requests․ Utilizing MSK MRI effectively requires careful consideration of patient history, physical examination, and established appropriateness criteria to optimize care․
5․3 Abdominal and Pelvic MRI: Organs and Structures
Abdominal and pelvic MRI provides detailed imaging of organs like the liver, kidneys, pancreas, spleen, and bowel, as well as pelvic structures including the uterus, ovaries, and prostate․ It’s valuable for detecting tumors, assessing inflammatory conditions, and evaluating congenital anomalies․ MRI offers superior soft tissue contrast compared to CT, making it ideal for characterizing lesions․
However, careful patient preparation is essential, often involving fasting and bowel preparation․ Consideration of contraindications, such as metallic implants, is paramount․ Appropriate utilization requires integrating clinical presentation with established imaging guidelines, ensuring MRI is the most suitable modality for the specific clinical question, optimizing patient-centered care․
5․4 Cardiac MRI: Heart and Blood Vessels
Cardiac MRI is a powerful non-invasive tool for assessing heart structure and function, visualizing blood vessels, and identifying areas of damage after a heart attack․ It excels at evaluating congenital heart defects, cardiomyopathies, and pericardial diseases․ Unlike other modalities, cardiac MRI doesn’t use ionizing radiation, making it a safer option for repeated scans․
However, cardiac MRI requires specialized protocols and expertise for image acquisition and interpretation․ Patient preparation often involves ECG gating and breath-holding techniques․ Judicious ordering, guided by clinical findings and appropriateness criteria, is crucial given the resource intensity and cost of this imaging modality, ensuring optimal patient care․
Optimizing MRI Ordering for Musculoskeletal Injuries
Musculoskeletal (MSK) MRI utilization demands careful consideration due to its frequent use and potential for overuse․ General practitioners (GPs) often initiate these referrals, highlighting the need for targeted training and quality assurance programs․ Guidelines focusing on appropriate MSK MRI utilization are essential to reduce unnecessary scans and associated costs․
Effective strategies include primary care-centric guidelines, educational initiatives for GPs, and feedback mechanisms on referral appropriateness․ Addressing uncertainty regarding direct access imaging pathways is vital; Prioritizing clinical correlation, physical examination findings, and a clear clinical question will significantly improve the value of MSK MRI scans, leading to better patient outcomes․
6․1 GP Training and Quality Assurance in MSK MRI Referrals
Addressing gaps in knowledge regarding appropriate MSK MRI ordering is crucial for primary care physicians․ Uncertainty exists concerning the effective use of direct access imaging pathways when managing musculoskeletal injuries․ Targeted training programs should focus on integrating clinical findings with established imaging guidelines, such as the ACR Appropriateness Criteria․
Quality assurance initiatives, including peer review and feedback on referral patterns, can further enhance appropriate utilization․ These programs should emphasize the importance of a thorough clinical evaluation before ordering an MRI, ensuring the scan is truly necessary for diagnosis and treatment planning․ Continuous medical education is key to improving referral quality․
6․2 Guidelines for Appropriate MSK MRI Utilization
Establishing clear guidelines for MSK MRI utilization is paramount for responsible healthcare spending and optimal patient care․ Judicious ordering, guided by clinical presentation and established criteria, minimizes unnecessary scans and associated costs․ Guidelines should prioritize MRI for cases where clinical examination suggests significant pathology, such as suspected ligamentous or meniscal tears, or bony abnormalities․
Emphasis should be placed on exhausting conservative management options – physical therapy, pain management – before resorting to MRI, unless red flags indicating serious underlying conditions are present․ Adherence to the ACR Appropriateness Criteria provides a framework for evidence-based decision-making, ensuring scans are ordered only when clinically justified․
Contraindications to MRI
Patient safety is paramount when considering MRI; therefore, understanding contraindications is crucial․ Absolute contraindications include the presence of non-MRI conditional pacemakers or implantable defibrillators, as the strong magnetic field can cause device malfunction and pose a life-threatening risk․ Ferromagnetic implants, like certain older aneurysm clips, also represent absolute contraindications․
Relative contraindications require careful evaluation․ Metal implants, even if not ferromagnetic, can cause image artifacts, potentially hindering diagnostic accuracy․ Pregnancy is a relative contraindication, particularly in the first trimester, due to potential, though unproven, risks to the fetus․
7․1 Absolute Contraindications: Pacemakers, Defibrillators
The presence of a non-MRI conditional pacemaker or implantable cardioverter-defibrillator (ICD) constitutes an absolute contraindication to MRI․ The powerful magnetic fields utilized in MRI can severely disrupt the function of these devices, potentially leading to life-threatening consequences such as inappropriate pacing or inhibition of defibrillation․
These devices contain metallic components that interact with the magnetic field, causing heating, movement, or reprogramming․ Even with newer, MRI-conditional devices, strict protocols must be followed, and a cardiologist’s clearance is essential․ Performing an MRI on a patient with a non-conditional device is unacceptable due to the significant risk of cardiac compromise․
7․2 Relative Contraindications: Metal Implants, Pregnancy
Certain metal implants represent relative contraindications to MRI, requiring careful evaluation․ While many modern implants are MRI-safe, older devices or those with unknown composition pose risks․ Ferromagnetic materials can heat up, move, or distort the image․ Thorough documentation of implant type and date is crucial․
Pregnancy is also considered a relative contraindication, particularly during the first trimester․ While MRI doesn’t use ionizing radiation, its effects on fetal development aren’t fully understood․ If MRI is deemed essential, alternative imaging modalities should be considered first, and careful risk-benefit analysis is paramount․ Gadolinium-based contrast agents are generally avoided during pregnancy due to potential fetal toxicity․
Preparing the Patient for an MRI Scan
Thorough patient preparation is vital for a successful MRI scan․ This begins with comprehensive screening questionnaires to identify any contraindications, like metallic implants or allergies․ Patients must disclose all medical devices and prior surgeries․
Specific instructions regarding medications are essential․ Some medications may interfere with image quality or patient safety; Patients should be advised about fasting requirements, if any, depending on the scan type and potential need for contrast agents․ Clear instructions regarding food and drink are also necessary to minimize movement and discomfort during the procedure․ Removing jewelry and wearing comfortable, non-metallic clothing is also crucial․
8․1 Patient Screening Questionnaires
Detailed patient screening questionnaires are the cornerstone of MRI safety․ These forms meticulously assess potential contraindications, focusing on implanted metallic devices like pacemakers, defibrillators, and certain aneurysm clips – representing absolute contraindications․ Questionnaires also explore relative contraindications, such as other metal implants, shrapnel, or pregnancy․
A thorough medical history is crucial, including prior surgeries, allergies (especially to contrast agents), and current medications․ The questionnaire must explicitly inquire about pregnancy status due to potential risks to the fetus․ Accurate completion and review of these forms are paramount to ensuring patient safety and preventing adverse events during the MRI procedure․
8․2 Instructions Regarding Medications and Food/Drink
Clear pre-scan instructions regarding medications and dietary intake are vital for optimal MRI image quality and patient comfort․ Patients should generally continue taking essential medications unless specifically advised otherwise by their physician or the radiology team․ However, certain medications, particularly those containing metal, may interfere with the scan and require temporary discontinuation․
Regarding food and drink, most MRI protocols do not necessitate strict fasting․ Patients are typically advised to eat and drink normally unless contrast agents are being used, in which case, fasting guidelines may apply․ Hydration is often encouraged to aid in contrast excretion․ Detailed, written instructions should be provided well in advance of the appointment to ensure patient compliance and a smooth scanning process․
Cost Considerations and Insurance Coverage
Understanding the financial aspects of MRI scans is crucial for both patients and providers․ MRI costs can vary significantly based on the body part imaged, the complexity of the scan, and the geographic location of the imaging center․ Patients should proactively inquire about the estimated costs before the procedure․
Insurance pre-authorization is frequently required by healthcare plans before an MRI can be covered․ It’s the patient’s responsibility to verify their insurance coverage and obtain any necessary pre-approvals․ Concierge services aim to eliminate insurance conflicts and scheduling hassles․ Failing to secure pre-authorization can lead to substantial out-of-pocket expenses․ Transparency in billing and clear communication with insurance providers are essential for a positive patient experience․
9․1 Understanding MRI Costs
MRI scan costs are multifaceted, influenced by several key factors․ The body part being imaged directly impacts price, with more complex regions like the spine or brain generally costing more than simpler scans․ The complexity of the protocol – whether contrast is used, or specialized sequences are required – also contributes to the overall expense․
Geographic location plays a significant role, with costs varying between states and even within cities․ Facility fees, technologist time, and radiologist interpretation all factor into the final bill․ Judicious ordering of MRI is essential for patient-centered care, considering the financial burden․ Patients should inquire about pricing upfront and explore potential options for cost reduction, such as freestanding imaging centers․
9․2 Insurance Pre-Authorization Requirements
Many insurance plans necessitate pre-authorization before an MRI scan will be covered․ This process involves submitting clinical documentation to the insurance provider, justifying the medical necessity of the imaging study․ Failure to obtain pre-authorization can lead to claim denials and significant out-of-pocket expenses for the patient․
Insurance requirements vary widely, with some plans requiring pre-authorization for all MRI scans, while others only mandate it for specific body parts or clinical indications․ Concierge radiology services aim to eliminate these hassles, streamlining the scheduling process․ Providers should be familiar with the specific pre-authorization guidelines of each patient’s insurance plan to avoid delays and ensure coverage․
Future Trends in MRI Ordering
The future of MRI ordering is poised for significant advancements, driven by the need for greater efficiency, cost-effectiveness, and patient-centered care․ Artificial intelligence (AI) and machine learning (ML) are expected to play an increasingly prominent role in optimizing imaging protocols and interpreting scan results․
Direct access MRI is likely to expand, empowering primary care physicians to order scans without referral, reducing wait times and improving access to care․ Emphasis on appropriateness criteria, like those from the American College of Radiology (ACR), will continue to grow, ensuring judicious utilization of MRI resources․ Tele-radiology will also become more prevalent, enabling remote interpretation of scans and expanding access to specialized expertise․